Blog
-

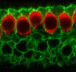
Team of Deaf Scientists probe hearing loss treatments. (The 10 faculty members in OHSU’s Oregon Hearing Research Center are considered trailblazers among their peers).
 30 Nov , 2016
30 Nov , 2016
At 14 months, he was struck with meningitis. The powerful antibiotic that saved his life largely stripped him of hearing.
His mother, determined to keep him in the hearing community, worked with him an hour a day for four years as part of an intensive regime of speech therapy. Sometimes it took him 10 minutes to learn a single word. He didn’t start to catch up to his peers until eight years later.
But today at 54, Steyger is a prominent auditory neuroscientist. At Oregon Health & Science University, he’s part of a team of researchers who are studying the auditory system in hopes of helping others who can’t hear.
“I look at their program as a very unique one in the world because of the breadth and the depth of their auditory science and the high quality of the science that’s done there,” said Jennifer Stone, an auditory neuroscientist at the University of Washington in Seattle.
The center also stands out in another way: It has five professors with hearing loss. Few other auditory research departments have even one scientist with a hearing disability. None has as many as OHSU, experts say.
Their varied biomedical backgrounds allow them to study every aspect of the auditory system, and their personal experiences inform their research.
“They’ve all got pretty high profiles and are covering lots of different bases,” said Jonathan Ashmore, a leading auditory neuroscientist based at University College London in Britain.
Their work has helped make the center, dating to 1967, one of the biggest nationwide. About a dozen other universities have hearing research centers with at least three faculty members. Only about five have 10 or more. OHSU’s department of otolaryngology – an ear, nose and throat specialty – is No. 2 in funding from the National Institutes of Health, at $10 million a year, right behind Johns Hopkins University.
For the scientists, it’s not been easy. Their hearing loss has complicated their lives. They struggled to follow their teachers and professors, keep up in graduate school and complete their post-doctoral training. They had difficulty taking notes. They suffered from a sense of isolation and found it tough to make friends.
But they found a home at the Oregon Hearing Research Center. They’re not alone in their disability, and they have a personal motivation to succeed. Though their research might not cure their own hearing loss, they hope to help the hearing of future generations.
“Each and every one of them had to work very hard to overcome the disabilities that they have but they’re all extremely effective communicators and very effective teachers,” Stone said. “Each and every one of them is a leader in their field.”
Steyger’s specialty is the toxicity of certain pharmaceutical drugs to the inner ear. He’s studying a powerful class of antibiotics called aminoglycosides, which are known to damage hearing.
Unlike some other antibiotics such as penicillin, which prevent bacteria from dividing, aminoglycosides kill bacteria. They include Gentamicin and Streptomycin, which Steyger was given for meningitis. He figures the antibiotic was responsible for his hearing loss or contributed to it.
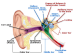
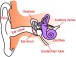
His Ph.D. thesis at Keele University in England, where he was born, focused on aminoglycoside-induced damage to the inner ear, which governs hearing and balance. In post-doctorate work at Keele, he studied the anatomy and function of the cochlea – part of the inner ear. When he got an offer from OHSU in 1997, he set up shop on the hill.
His lab is trying to understand how aminoglycosides cross the blood-labyrinth barrier, which has a similar function to the blood-brain barrier but instead of protecting the brain, it protects the ears from harmful substances. Aminoglycosides exploit an existing pathway for other compounds, allowing them to barge through the physical barrier.
Both infections and aminoglycosides can harm hearing by themselves, and in a triple whammy effect, the inflammation that’s caused by an infection allows more of the antibiotics into the inner ear. Steyger is trying to understand the mechanics of how that happens.
“This is a serious issue, and it’s not just affecting me,” he said. “It’s still affecting people today.”
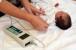
Eighty percent of premature babies who enter a neonatal intensive care units get antibiotics to prevent infections, Steyger said. If they’re kept on them long enough, they can lose their hearing.
“When a kid is born, if they’re not treated with aminoglycosides and they have an infection, they can die within 12 hours,” Steyger said. “That’s why so many kids will get the drug.”
His choice to focus on hearing was strategic, he said.
“I expected that they would be more welcoming of a hearing-impaired person,” said Brigande, 51. “The annual meetings would have captioning. They would have listening technologies. I thought that this would be an obvious, clear path to give me the best chance to communicate effectively.”
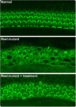
At OHSU, he’s working with mice that are congenitally deaf. He’s found a way to introduce a healthy gene into the inner ear while the animal is in the womb. When they’re born, they can hear.
“John’s a superstar,” Ashmore said. “That really is a technical discovery of the first order.”
Brigande wants to see his work benefit people.
“I’m passionately committed to trying to make that happen,” Brigande said. “I would love to be able to spare a child from growing up with hearing loss.”
Besides breaking new ground in the lab, Brigande has raised awareness about the need to accommodate students with hearing impairments on the campus. Together with Steyger, he’s persuaded OHSU management to equip conference halls with assisted-listening devices.
The center’s director, Alfred Nuttall, 73, whose hearing loss started in his 40s, said their personal situations didn’t influence the decision to hire Steyger, Brigande and Lina Reiss, who’s 41 and another member of the department with severe hearing loss. Frederick Gallun, 45, originally hired by the VA Portland Health Care System, also conducts auditory research at the center and can hear out of only one ear.
“Every scientist we have hired is based on the science that they’re working on – not their hearing loss,” Nuttall said.
During the first 48 hours, a blood test is done to determine whether they have an infection. If not, they’re taken off the drug, usually without consequences, he said. But if they have an infection, they’re kept on the medication.
“Once you start giving children drugs for more than five days, the chances of them getting hearing loss from the drug starts to increase dramatically,” Steyger said.
He estimates that 35,000 children a year nationwide suffer some degree of hearing loss because of the antibiotics. He hopes to find a way to block aminoglycides from entering the inner ear.
“If we can stop them from crossing the barrier, we can preserve the hearing that we already have,” Steyger said. “If we can preserve that that, it will be much better than any regeneration strategy that exists at present.”
Another researcher at the center, John Brigande, is focused on preventing deafness through treatments in the womb.
Like Steyger, Brigande has profound hearing loss. He gradually lost hearing in his left ear from some unknown cause. By the time he was in college, he had to wear hearing aids. He ended up doing post-doctoral training with a hearing scientist at Purdue University in Indiana in an environment that accommodated his disability.
But having them all has turned out to be an advantage for the scientists. It creates camaraderie and boosts their confidence in their work.
“It’s very stimulating to be around a group with many deaf people,” Reiss said.
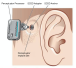
Her lab is trying to understand why some people with hybrid cochlear implants – which combine an implant with a hearing aid in the same ear – do well while others don’t. Steyger, who has a traditional cochlear implant, takes a keen interest in her work, feeding her hypotheses to test.
During his first six years at the center, Steyger was the only one with profound hearing loss. Now that he’s not alone, he enjoys a sense of community.
When he first arrived, he said he often wondered whether he was there as the token faculty member with hearing loss.
Then OHSU hired Brigande, followed by Reiss. Today they all need hearing aids to do their ground-breaking work.
“Our field’s been redirected by these individuals,” Stone said. “They’ve highlighted new questions. They’ve taken the research in new directions and that’s influenced people to follow.”
Source: LYNNE TERRY KSBW News, Portland Ore.
Image credit : OHSU’s Oregon Hearing Research Center