Blog
-

Acoustic Shock… by Nail Gun (Dennis Colucci, PhD)
 15 Apr , 2016
15 Apr , 2016
Acoustic shock (AS) is a rare condition caused by an unexpected loud sound and resulting in a number of otologic symptoms, including otalgia without physical findings, tinnitus, hyperacusis, mild dizziness, and, in some cases, tonic tenor tympani syndrome and trigeminal nerve irritability.
Acoustic shock is a life-changing disorder with a significant psychogenic component. People suffering from AS often stop working, retreat into isolation, and use hearing protection insidiously, as they fear everyday sound. What appears initially to be a complaint of peripheral hearing loss and tinnitus is actually much more extensive, as the central auditory structures and the limbic system become engaged and the patient’s behavior
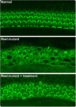
According to Lin et al., neuropathic changes to the cochlear nerve peripheral terminals and a slow degeneration of spiral ganglion cells occur in animals that are acoustically overstimulated, even in the absence of inner or outer hair cell loss, with the recovery of hearing thresholds (Lin. J Assoc Res Otolaryngol 2011;12[5]:605–616) Additionally, Hickox et al. report that an acoustic insult can create neural alterations that result in maladaptive neuroplasticity.Furthermore, these changes result in central neural hyperactivity, which initiates and maintains chronic tinnitus and hyperacusis. From these and other studies, it is clear that acoustic shock and noise trauma produce higher-order changes that go far beyond the audiogram.
The AS incident that causes tinnitus and the reaction to sound is loud, startling, novel, and unpredictable. Furthermore, it produces unexpected discomfort and pain, making the individual feel anxious. Following the “shock,” daily activity can center on chronic tinnitus awareness and annoyance, along with an avoidance approach to everyday sounds. With no treatment and resolution in sight, this promotes a downward spiral of psychological impairment, including distress, depression, social detachment, thoughts of suicide, and self-pity.
AN EXAMPLE OF SUCH AN INCIDENT AND IT’S RESULT.
THE CASE OF THE CONSTRUCTION WORKER
A 54-year-old patient reports being in good health with a negative medical history, including the absence of hearing loss; tinnitus; vertigo; head, neck, or barotrauma; or socioacusic activities prior to the incident.
The subject had been a construction worker for 25 years, primarily building offices and manufacturing space, using nail guns throughout his career. The patient reports using hearing protection, but one day he used a pneumatic nail gun (109–136 dBA), without using protection, in a ceiling corner of a 10 × 10 × 10 concrete enclosure.
He had worked for only a few minutes when the sound became excruciatingly loud and he immediately stopped working. He felt pain, had sound quality discomfort, and immediately became anxious. Within a few hours, the patient developed tinnitus; within a week, he complained of sound tolerance issues. This developed into debilitating tinnitus and hyperacusis, with symptoms of tonic tensor tympani syndrome, within a few months. Subsequently, he went on medical leave and eventually retired.
The patient has started using earmuffs for all listening conditions, including in his home, claiming that normal sound—including his own voice, television, and conversation—hurts or is irritating. He is unable to obtain adequate treatment or manage his debilitating conditions and resorts to isolation, complaints of depression, and has passive thoughts of suicide.
The patient’s pure tone air and bone conduction thresholds reveal a mild to moderate high-frequency sensorineural hearing loss, with 4K Hz notching in both ears. Recorded speech reception thresholds and speech discrimination scores are within normal limits, bilaterally. Admittance testing reveals type A tympanogram, bilaterally. UCL measures for octave frequencies between 250 and 4000 Hz are between 65 and 75 dB in either ear.
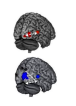
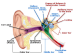
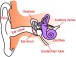
Changes in plasticity created by acoustic trauma go far beyond damage to the OHCs and hearing loss. They start with the IHC and cochlear nerve terminals and more rostral connections, such as the dorsal cochlear nucleus and inferior colliculus and beyond. Moreover, these changes can trigger central neural hyperactivity, producing tinnitus and hyperacusis.
In cases of AS, the patient history and circumstances of the incident are paramount. Understanding the central effects and affects provide a groundwork for patient diagnosis and management. Treatment for the AS patient should start immediately with a team, including otology, psychiatry, psychology, neurology, and audiology specialists. The psychopathology must be addressed at the onset.
Source: Copyright © 2016 Wolters Kluwer Health, (Courtesy of The Hearing Journal. 69(4):48, April 2016).
Image credit: Dennis Colucci, PhD